Rotator Cuff Surgery Overview
Orthopaedic Specialists 502-212-2663
Stacie Grossfeld, M.D. / Bess Fley, PA-C
Preparation For Surgery; The Night Before
- Rotator cuff surgery is performed as an outpatient procedure.
- Do not eat or drink after time given by Dr. Grossfeld’s staff
- Wear loose-fitting clothing
- Bring Insurance information and picture ID
- List of medications and drug allergies
- Arrange for someone to drive home after procedure
Upon arrival at the surgery center you will first meet with the registration person to check you in. You will then be brought back to the pre-op area and meet with your nursing team. Vital signs, such as blood pressure and temperature, will be measured.
A clean hospital gown will be provided. All jewelry, dentures, contact lenses, and nail polish must be removed. An IV will be started to give you fluids and medication during and after the procedure. Your shoulder will be scrubbed and shaved in preparation for surgery. An anesthesiologist will discuss the type of anesthesia which will be used. Dr. Grossfeld will confirm and initial the correct surgical site with a marking pen.
Anesthesia
Prior to the procedure you will meet the anesthesiologist. At that time, they will discuss your medical/past anesthesia history with you. The anesthesiologist will place a nerve block to numb your shoulder and arm. The numbing medicine will last for 18 hours. This is a great way to reduce post operative pain. Even after the nerve block wears off, your pain level is reduced because of the anti-pain effect of the nerve block.
After the nerve block is placed, you will go to the operating room where the surgery is performed. The anesthesiologist will administer a general anesthesia, so you are completely asleep for the procedure. You will not hear or see anything going on in the operating room.
Surgical Procedure
Dr. Grossfeld will perform the rotator cuff repair arthroscopically. This procedure takes between 45-90 minutes. After you head back to the operating room it takes about 40-50 minutes to go to sleep and get positioned on the operating room bed, so your family may not see you for 2.5 hours depending on how extensive the surgical procedure. Dr. Grossfeld will make five to six small incisions that are less than a ½ an inch in length around the shoulder joint. A small high-definition camera, about the size of a pencil, will be placed into the shoulder joint. After the camera is inserted, inspection of the whole shoulder joint is completed. Each compartment of the shoulder is viewed. The location of the rotator cuff tear will be identified. If there are any bone spurs those will be removed. Removal of the bone spur is called a subacromial decompression, and/or an AC joint excision. Any other abnormal findings will also be addressed at the time of the surgery and repair.

The repair of the rotator cuff is done by placing three or four suture anchors into the shoulder bone.
Suture anchors are made out of a synthetic bone, the anchors will incorporate into your own bone. The image to the left is a suture anchor used to repair torn rotator cuffs.
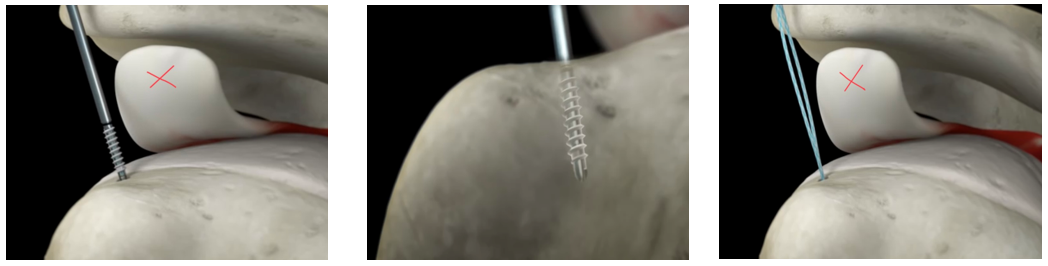
The first image above reveals the anchor being screwed into the shoulder bone (the x marks the torn rotator cuff tendon). The middle image shows the suture anchor secured into the shoulder bone. The last image shows how the sutures are now “anchored” into the humerus and ready to be sutured through the torn rotator cuff tendon.
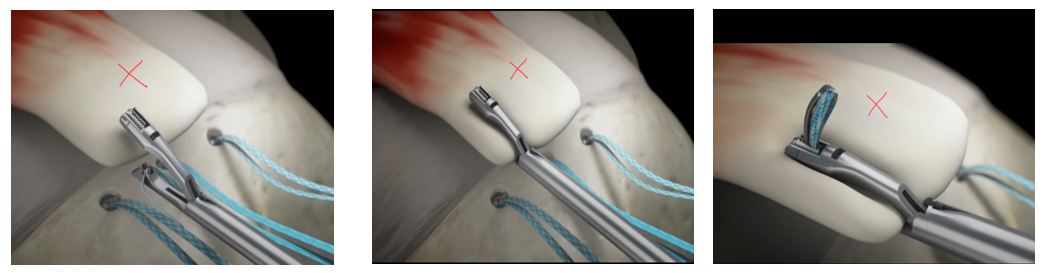
The images above show how the suture is sewn through the torn rotator cuff tendon. The sutures are pasted through the torn rotator cuff tendon with a special instrument designed specifically for the task.
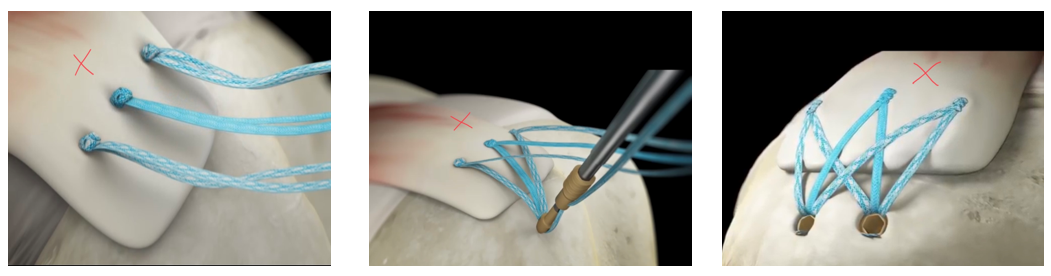
The three images above show the knots that are tied to hold the torn tendon against the shoulder bone. The second and third image show the second set of anchors that reinforce the repair. The final picture is a repaired rotator cuff tendon.
The repaired tendon will be reattached to the bone. The sutures are there to hold the tendon securely up against the bone while the healing process takes place.
If there are any bone spurs, they will be removed with a small tool that similar to a Dremel.
The incision site/portal sites are closed with a blue colored suture called Prolene. The sutures will be removed when you are seen in the office at 10 to 14 days post-surgery.
Upon leaving the operating room, you will have 4 x 4 gauze placed over the incision sites followed by ABD pads which are a larger fluffy dressing, followed by surgical tape. Your specialized shoulder sling will be fitted in the operating room.
You will get a detailed set of instructions on wound care upon discharge from the surgery center.
Night of Surgery
It is very important you stay on top of the pain. Ice is key. Use ice as MUCH as possible. Dr. Grossfeld recommends continuous use of ice around the clock. The rule is you cannot use too much ice. Whether it is a Polar Care unit or bags of frozen peas: use it continuously for 6-7 days after surgery.
Polar Care units are available for purchase Orthopaedic Specialists for $150.00. They are not covered by insurance. Polar Care is a motorized ice machine which consist of a neoprene wrap that gets placed over the operative shoulder and a cooler that is filled with ice and water. A hose connects to a neoprene wrap that goes around the shoulder, and will push water through the neoprene wrap for up to nine hours. Please freeze eight water bottles before your surgery. Put four frozen water bottles into the Polar Care unit. Then, fill with water. This will keep the with water colder longer. When the four water bottles defrost, replace with four more frozen bottles and put the defrosted bottles back into the freezer. Continue to repeat this cycle. Use ice around the clock, even when sleeping. Ice is the best source of pain control and swelling.
Set your alarm clock and take your pain medication every 4 to 6 hours for the first 24 hours to stay on top of your pain. Adding 800 mg Motrin every 6 hours OR Meloxicam 15 mg every 24 hours can also help to reduce post operative pain. Do not use Motrin or Meloxicam if you are on blood thinner or have a history of stomach ulcers or kidney disease
Sleeping in a recliner, in an upright position, or using lots of pillows to support your shoulder will be more comfortable. Some people will sleep in a recliner for up to 4 weeks after surgery. Lying flat in bed allows your shoulder to roll back which tugs on the repair, and will cause pain.
Sling Use
You will wake up in the recovery room with your sling on. Occasionally you may take the sling off while at rest, (NOT asleep), as long as you place your arm against your belly. When asleep the sling must be on.
Surgical Dressing
A dressing, consisting of 4×4 gauze pads, ABD pads and special surgical tape will be placed on the surgical site(s). Please refer to your post operative orders given to you the day of surgery for dressing change details.
Dressings to purchase before your surgery day are: 10-15 4×4 gauze pads, an extra 6-inch ace wrap, peroxide, paper tape and waterproof Band-Aids. Kits are available for purchase at Orthopaedic Specialists.
First Post-Operative Visit
Your first post operative visit will be 10-14 days post-surgery. Sutures will be removed by an assistant. Dr Grossfeld or Bess Fley, PA-C will go over your operative report, surgical photos, and answer any remaining questions. Physical therapy may be ordered. Typically, physical therapy is only once or twice a week for the first six weeks. PT will vary from person to person based on the size of the tear and repair quality.
Home Exercises & Physical Therapy
Exercises will be given to do post op. A link to these exercises is on the post operative instructions/orders given the day of your surgery. The link will show you how to do some gentle post operative exercises. A set of pulleys, which can be purchased from our office for $20, allow you to work on passive range of motion exercises at home after the surgery.
Physical therapy is divided into three 6-week blocks. The first 6 weeks you will attend once a week to work on gentle passive range of motion exercises.
The second six weeks therapy involves active range of motion of the shoulder with some gentle strengthening. You will attend 1-3 times a week, depending on your repair and other factors.
The third six weeks of physical therapy involves increasing range of motion and further strengthening. This is about a five-to-six-month recovery before you are back to your normal activities involving the operative shoulder.
Driving
You may begin to drive after you’re off all narcotic pain medications. Once you begin driving your sling needs to be taken off while driving. It is recommended you place your hand, of the operative side, at the bottom of the steering wheel and your non-surgical hand at the top of the steering wheel to do most of the work.
Return to Work
If you work a labor type job, you may not return until you are released 100%. However, if your employer can accommodate light duty options you may return as soon as two to four weeks after surgery. Light duty options require no use of the surgical extremity, except for simple tasks such as using a computer.
If you have an office type job, you can most likely get back to work between two to four weeks. Return to work also is dependent upon pain level. Some people have a lot of pain after this particular surgery, some people have very little. Pain is very personal, and we will supply you with pain medication in accordance to our office policy and Kentucky state law. Pain medication will be prescribed appropriately in regards dosages, amount, and time.
FMLA and Disability Paperwork
Our office offers the service of completing paperwork for FMLA and/or disability for a fee of $40, per set of paperwork, and is completed in the order that it is received, typically takes 7-10 business days. All requests must originate with your employer, as your eligibility for FMLA and/or disability is based on your benefits with your employer. While each patient is unique, we do our best to estimate the time of recovery and often times over-estimate the amount of time to prevent a lapse in benefits and/or require additional paperwork. Often times disability companies require updates after each appointment. It is the patient’s responsibility to communicate this request with the office. Updates are not automatically completed. Any questions regarding this can be directed to Dorothy.

Recent Comments