Key Takeaways:
- A Mayo Shear Test is a noninvasive motion test that can help to identify labral tears in the shoulder.
- If a labral tear is present in the shoulder, the patient will normally feel pain in the back of the shoulder and/or hear a clicking sound.
- A labral tear occurs when the specialized cartilage tissue in the shoulder is torn or damaged, usually from throwing, pushing, or doing overhead tasks.
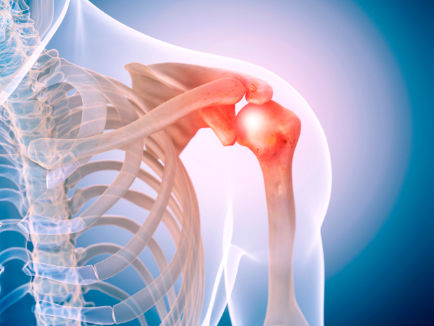
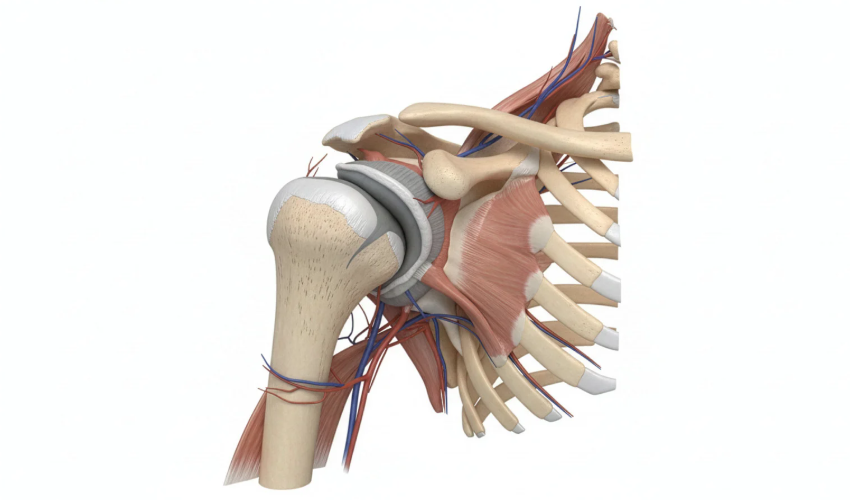
The labrum is a special piece of cartilage that cushions the ball-and-socket joint of the shoulder. This joint is made up of the humeral head from the arm (the ball) and the glenoid (the socket). The labrum lives on the rim of the glenoid and serves as an attachment location for the ligaments that connect the humerus and and the glenoid.
How Do You Know If You Have a Torn Labrum in Your Shoulder?
Damaged or torn labrums often result from either acute trauma or repetitive shoulder motion (OrthoInfo). In many cases, this leads to shoulder pain (especially with overhead activities), shoulder instability, and other symptoms such as:
- Dislocations
- Sensations or noises of catching, locking, popping, or grinding
- Increased shoulder pain at night
- Decreased range of motion
- Loss of strength
There are three types of labral tears that are most common:
- SLAP Lesion – a tear that occurs on the upper part of the socket. This kind of tear also affects the bicep tendon.
- Bankart Lesion – a tear that occurs at the bottom of the socket. This normally results from a shoulder dislocation.
- Posterior Labrum Tear – a tear that occurs at the back of the socket. Wear and tear or acute injuries are commonly the culprits for this type of tear.
If you play a sport that involves a lot of throwing or a similar motion to it, or your daily activities require you to repetitively lift heavy objects, your shoulder pain might be a torn labrum. The only way to determine with any certainty that you have torn your labrum is with imaging tests like CT scans or MRIs. However, in order to narrow down the possible origin of your shoulder pain, doctors may perform simple, non-invasive movement tests like the Mayo Shear Test.
How To Do a Mayo Shear Test
For this labral tear of the shoulder test, you will:
- Adduct the affected arm
- Bend the elbow so the arm is at 90 degrees with the arm externally rotated and your hand on the back of their shoulder
- Bring up to about 120 degrees of forward flexion
- Then pull the arm down to about 60 degrees
If the up and down movement produces a click or other noise, and produces pain along the posterior (back portion) of the shoulder, they may have a labral tear, usually a Bankart lesion or posterior labrum tear.
Frequently Asked Questions About Labral Tears in the Shoulder
- Will a torn shoulder labrum heal completely?
- If the tear is mild and proper steps to rehabilitation is followed, most patients will have full function of the shoulder and return to their activities with few or no restrictions. In the case of Burkart lesions, some patients report feeling like their shoulder will dislocate again. Focusing on rebuilding the muscles of the shoulders will be very helpful for stabilization.
- Can a labral tear in the shoulder heal on its own?
- In some cases, conservative treatments like rest, over-the-counter pain killers, and physical therapy can be enough to heal a labrum tear. However, it is not recommended that no action be taken, as this will increase the possibility of reinjury, or worsening the tear.
- How do you fix a labral tear in the shoulder?
- Common treatments for shoulder labrum tears include activity restrictions, physical therapy, anti-inflammatory medication, corticosteroid injections for pain management, or in more severe cases, shoulder arthroscopy surgery to trim or reattach the labrum to the glenoid.
- How long does it take to recover from a labrum tear in the shoulder?
- Without surgery, this will vary case-by-case. Healing can be unpredictable due to factors like how rigidly the patient adheres to a recovery plan and how severe the tear is. With surgery, there is more structure, and patients usually have a minimum recovery period of 12 weeks, but it will take 4-6 months to return to activities at full-strength.
If you or someone you love has suffered a shoulder labrum tear in the Louisville, Kentucky-area, board certified sports medicine physician Dr. Stacie Grossfeld at Orthopaedic Specialists PLLC can help. Orthopaedic Specialists PLLC is accepting new patients, and same day appointments are available. For additional information or to schedule an appointment, please contact Orthopaedic Specialists PLLC today at 502-212-2663.











Recent Comments