
Key Takeaways:
- Even if arthritis looks bad on an x-ray, you don’t always need a total knee replacement surgery.
- Knee replacement should be a last resort after all conservative treatments fail to help manage pain.
- Common conservative treatments include hyaluronic acid and cortisone injections, physical therapy, and topical anti-inflammatory medications.
When we see x-rays, it can be easy to draw the worst conclusions if a condition like arthritis looks bad on a scan. Severe arthritis, also known as late-stage, grade 4, or bone-on-bone arthritis, is one of these. Arthritis affects over 53 million US adults (CDC), and one of the treatments available is a total knee replacement. If you see bone-on-bone arthritis in your x-ray scans, does that mean you need a knee replacement surgery?
The good news is that the answer is: not always!
When Do You Need a Knee Replacement?
While x-rays can help us to diagnose and track conditions like arthritis, treatment is not so straightforward as other medical issues like a broken arm. Treating chronic conditions like arthritis depend a lot on how the patient feels, not what their x-ray looks like.
If someone breaks their arms, and it shows up on an x-ray, then there is a process to heal it. Arthritis cannot be healed, only managed. And, the pain that should be managed is the pain that the patient feels, not whatever an x-ray shows, necessarily. If a patient is doing well with conservative treatments, surgery should not be recommended lightly, if at all.
Knee replacement surgery should only be a last resort, when nothing else works. If the patient has done all they can and still finds their daily activities to be interrupted by pain from arthritis, then knee replacement might be the next step.
Non-Surgical Treatments for Severe Arthritis of the Knee
Conservative, or non-surgical, treatments for severe arthritis of the knee are aimed at mitigating symptoms, not curing the condition. Arthritis is not a condition that can be cured. At Orthopaedic Specialists, our most common non-surgical treatments for arthritis include:
Hyaluronic Acid Injections
Hyaluronic acid is a naturally occurring fluid in your body that cushions your joints and fuels your skin, eyes, and connective tissues. Arthritis can cause it to deteriorate. Injections can replace that deteriorating fluid and add supplementary lubrication to your joints to help with pain and movement.
Cortisone Shots
Cortisone shots, or corticosteroid injections, are anti-inflammatory medications that are injected directly into arthritic or painful areas of your body. Because some forms of arthritis, like rheumatoid arthritis, are caused by an inflammatory response in your body, this injection can help mitigate pain in 2-5 days.
Physical Therapy
Many people might not realize that physical therapy isn’t only for injury rehabilitation. Seeing a specialist who knows about body movement and mechanics can help you learn how to move with less pain. Engaging the muscles around joints can strengthen them and help take some of the load off of the afflicted joint.
Daily Exercise
In addition to physical therapy, daily exercise works to help in the same way. Strengthening your body helps to reallocate how you bear weight. Muscles are just as important as joints, and play a huge part in keeping them safe. Low-impact activities like riding a spin bike, walking, swimming, and yoga are all recommended exercises for knee pain.
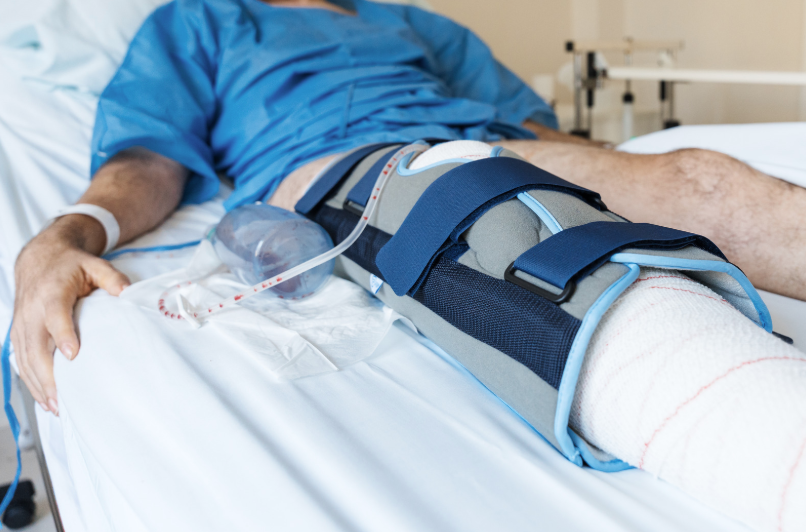
Unloader Knee Brace
An unloader knee brace can help you resume activities that may otherwise be too painful to do with severe knee arthritis. It provides levels of compression, stabilization, and weight redistribution to help unload the side of your knee that is affected by arthritis. There are a few types of unloader braces. You should consult with your doctor to discuss which type would be best for your pain.
Topical Anti-inflammatory Gel
Topical anti-inflammatory medications come as creams or gels that are applied to the skin around painful joints. The medication then soaks into the skin. Because of this, topical anti-inflammatory medications are best used on joints close to the skin, like the knees, hands, and wrists. Common medications you’ll see are Diclofenac sodium (Pennsaid, Voltaren) and Triamcinolone (Kenalog, Triderm).
Frequently Asked Questions About Knee Replacement Surgery
- How long does it take to recover from knee replacement surgery?
- Recovery time will depend on factors like age, health, and rehabilitation adherence. However, most patients go home the day or the day after their surgery, regain mobility by three months, and recover fully within a year (Penn Medicine).
- How long will a knee replacement last?
- A knee replacement can last up to 20 or 30 years if taken care of properly. Those who are more active may wear their replacement out faster.
- What is the difference between a total knee replacement and a partial knee replacement?
- The knee joint comprises three areas: medial, lateral, and patella. In a partial knee replacement, a surgeon will replace one or two of these areas. In a total knee replacement, they will replace all three areas.
If you or someone you love suffers from severe arthritis of the knee in the Louisville, Kentucky-area, board certified sports medicine physician Dr. Stacie Grossfeld at Orthopaedic Specialists PLLC can help. Orthopaedic Specialists PLLC is accepting new patients, and same day appointments are available. For additional information or to schedule an appointment, please contact Orthopaedic Specialists PLLC today at 502-212-2663.











Recent Comments