 Last week, Orthopaedic Specialists published an article entitled “The ABCs of Orthopedics: Part 1” that listed common terms related to orthopedics. We covered letter A – M and are back this week to complete the list in Part 2.
Last week, Orthopaedic Specialists published an article entitled “The ABCs of Orthopedics: Part 1” that listed common terms related to orthopedics. We covered letter A – M and are back this week to complete the list in Part 2.
We hope that by defining 26 common terms used in the study of orthopedics, we will help patients become familiar with verbiage and more relaxed. Dr. Stacie Grossfeld strives to have a relaxed and comfortable office environment at both of her Louisville, KY locations. Familiarity with terms used by office staff can often remove the edge of nerves induced by an office visit. So, without further ado, we present the second installment of the ABCs of Orthopedics as defined by Dr. Stacie Grossfeld.
The ABCs of Orthopedics: Part 2 (N-Z)
N is for Neuropathic Arthritis
More commonly known as “Charcot foot”, neuropathic arthritis is the degeneration of a weight bearing joint. Neuropathic arthritis often results in a bony obstruction and deformity. There are many reasons that one can develop neuropathic arthritis including: diabetes, leprosy, syphilis, a spinal cord injury, or peroneal muscular atrophy. Despite all the causes, diabetes is the leading cause in America and the foot is the most commonly affected part of the body.
O is for Osteoporosis
Bone health is extremely important for orthopedic surgeons and their patients, but unless you’ve recently suffered a bone injury then it’s safe to say you don’t really think about your bones. However, osteoporosis – the degradation of bones – affects over 50 million Americans with one in two being women and one in four being men.
P is for Pediatric Orthopedic Injuries
Unfortunately, pediatric orthopedic injuries are common and most often include: wrist sprains, femur fractures, trampoline injuries, winter sports injuries, and broken clavicles. While pediatric orthopedic injuries are scary for parents and children alike, they are easily treatable and often heal without any issues arising.
Q is for Quadricep Tendon Ruptures
Quadricep tendon ruptures are classified as a sport injury and most often occur in football players. Interesting studies done by the AJSM looked specifically at injuries in the NFL and specifically reviewed quadricep tendon ruptures. Both studies found that men who used steroids were much more likely to rupture their quadricep tendons. Diabetes, renal failure, RA, and infections could also predispose players to ruptures.
R is for Rotator Cuff Repair
The rotator cuff is a part of your shoulder that allows you to move your arm in a full circular motion without pain. However, often due to injury or overuse, it is crucial that the rotator cuff undergo repair. Rotator cuff repair is a common surgery performed by orthopedic specialists like Dr. Stacie Grossfeld and she specializes in rotator cuff repair performed arthroscopically.
S is for SLAP Tear
A SLAP tear is a term for a common shoulder injury that refers to a tear or rip in the labrum. The labrum is the tissue that surrounds and protects your shoulder socket and when it is torn, it is referred to as a SLAP tear which stands for Superior Labrum Anterior to Posterior. SLAP tears are common injuries among people who often lift heavy things or exercise a lot of repetitive overhead movements. However, SLAP tears can also occur when a person falls on their shoulder or when someone braces themselves during a car crash.
T is for Tendinitis
Tendinitis occurs when the tissue that connects bone to muscle inflames and affects the area in which it has swelled. There are different types of tendinitis that focus on different areas of the body. Most often they are named after the sport that is most commonly the cause of the inflammation. Examples include “tennis elbow” and “golfer’s elbow”; however, tendinitis can affect other areas of the body including the knees, shoulders, calves, and wrists.
U is for Ulnar Collateral Ligament Injury
An ulnar collateral ligament injury is similar to an ACL injury. However, UCLs affect elbows and are an injury that commonly affects the throwing athlete. Repetitive forces to the elbow from throwing tend to place abnormal stress on the joint and predispose athletes to acute injuries. However, like a torn ACL, a torn UCL can be fixed through reconstructive surgery.
V is for Voluntary Muscle
A voluntary muscle is a muscle that can be controlled by will and is attached to the skeleton. You can often identify a voluntary muscle because it is one that can be worked out through strength training exercises. Voluntary muscles include: quadriceps, biceps, pectorals, etc. In contrast to voluntary muscles, your body is also made of involuntary muscles that do not need to be controlled, but instead simply work on their own accord. A perfect example of a involuntary muscle is the heart which is often thought of as an organ, but is in fact a muscle.
W is for Weight Loss
Body weight affects health much more than most people are aware of. Being overweight, or obese, can have negative effects on your bones, muscles, joints, and organs. Weight loss is a great way to maintain your health. Often, for someone who is in need of a total knee replacement or other repair, weight loss is required to become an eligible surgical candidate. At Orthopaedic Specialists, we want our clients to live the best and healthiest lives they can which often starts with weight loss and exercise.
X is for Lower Extremity Avulsion Fractures
Lower extremity avulsion fractures are common injuries in pediatric and adolescent patients. This is because youths have growth plates that are still open and connected to tendons. When a traumatic event happens to areas of the body, often the plate suffers an avulsion fracture.
Y is for Youth Sport Specialization
What is considered as sport specialization? According to Dr. Brian Feeley, youth sport specialization is year-round, intensive training in a single sport. However, Dr. Feeley is also concerned that youth sport specialization at a young age increases the rates and risk of overuse injury and burnouts mentally. This can be especially true for youth athletes who start specializing in a single sport at a young age with a large group of peers. Some sports that fall into this category and should be monitored for overuse injuries include: cheerleading, gymnastics, football, and baseball.
Z is for Zika Virus
The Zika virus gained attention after the media started covering it after it started spreading at a fast rate. However, the Zika virus has been a concern since the 1950s in Central and South America. Due to the seriousness of the virus, it is important people are aware of symptoms. Symptoms include: headaches, rash, fever, joint and muscle pain. Conjunctivitis is also a main symptom of the Zika virus that can be a telltale sign if one is confused on what their symptoms mean. While there are no vaccinations against the virus, acetaminophen will help manage the pain until it passes. Once a person is infected with the virus, they are protected against future infections.
At Orthopaedic Specialists, we strive in making our patients and office visitors as comfortable as possible. We know that the medical field can be overwhelming and confusing. This is why we work so hard to achieve transparency between our office staff and patients. We hope these two installations of the ABCs of Orthopedics help to alleviate some confusion.
Dr. Stacie Grossfeld at Orthopaedic Specialists in Louisville, KY has over 20 years of medical experience. If you are suffering from bone, joint, or muscle pain or have experienced a sports-related injury, contact her today. You can contact Orthopaedic Specialists by calling 502-212-2663 or filling out a contact form.


 If every school had an athletic trainer as dedicated, knowledgeable and passionate about their work, there’s no doubt the number of youth sports injuries would significantly drop, while the overall athletic performance would noticeably increase. But Kelly Dike is one of a kind and it’s certain that very few school athletic programs have an athletic trainer as dedicated and experienced.
If every school had an athletic trainer as dedicated, knowledgeable and passionate about their work, there’s no doubt the number of youth sports injuries would significantly drop, while the overall athletic performance would noticeably increase. But Kelly Dike is one of a kind and it’s certain that very few school athletic programs have an athletic trainer as dedicated and experienced. After graduating from high school, Kelly attended
After graduating from high school, Kelly attended 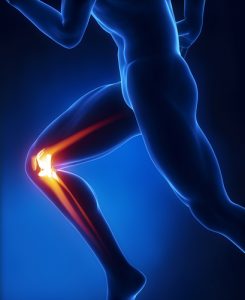 Dr. Stacie Grossfeld is a double board-certified surgeon in the fields of orthopedic surgery and also sports medicine. Her combination of specialties means that she spends a lot of time working with injured athletes around Louisville, KY. One of the most common injuries among high school and college athletes are torn Anterior Cruciate Ligaments (ACLs). In order to offer the best medical care that she can, Dr. Grossfeld stays up-to-date on scientific findings surrounding
Dr. Stacie Grossfeld is a double board-certified surgeon in the fields of orthopedic surgery and also sports medicine. Her combination of specialties means that she spends a lot of time working with injured athletes around Louisville, KY. One of the most common injuries among high school and college athletes are torn Anterior Cruciate Ligaments (ACLs). In order to offer the best medical care that she can, Dr. Grossfeld stays up-to-date on scientific findings surrounding  Pregnancy is a miracle in and of itself; however, that doesn’t mean that the entire process is painless. For most women, the excitement of bringing a child into the world overpowers any discomfort. That is not the case for everyone though. Some women find themselves in quite a bit of pain while pregnant. One of the most common causes of pain in women who are pregnant is backache. Other causes of pain and discomfort include:
Pregnancy is a miracle in and of itself; however, that doesn’t mean that the entire process is painless. For most women, the excitement of bringing a child into the world overpowers any discomfort. That is not the case for everyone though. Some women find themselves in quite a bit of pain while pregnant. One of the most common causes of pain in women who are pregnant is backache. Other causes of pain and discomfort include: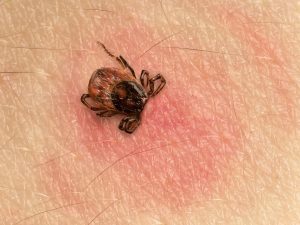
 While eating nutritious foods and working out are great ways to improve your health, there is so much more to consider. Health and wellness requires a holistic approach that not only focuses on nutrition and fitness, but other areas as well. In order to achieve optimal health, it may be worth your while to take a look at the 15 habits of healthy people.
While eating nutritious foods and working out are great ways to improve your health, there is so much more to consider. Health and wellness requires a holistic approach that not only focuses on nutrition and fitness, but other areas as well. In order to achieve optimal health, it may be worth your while to take a look at the 15 habits of healthy people. ACL stands for Anterior Cruciate Ligament and this part of the human body runs between the femur and the tibia. It is one of a pair of cruciate ligaments in the human knee. The other is the Posterior Cruciate Ligament which is located deeper within the knee joint. When an ACL is injured, or torn, it is due to the ligament being overstretched. Most often,
ACL stands for Anterior Cruciate Ligament and this part of the human body runs between the femur and the tibia. It is one of a pair of cruciate ligaments in the human knee. The other is the Posterior Cruciate Ligament which is located deeper within the knee joint. When an ACL is injured, or torn, it is due to the ligament being overstretched. Most often,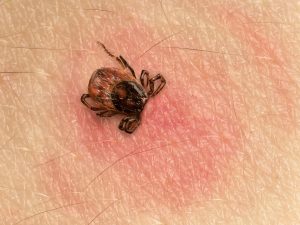 Lyme disease is a bacterial infection that is transmitted by Ixodes ticks, more commonly known as deer ticks. These nymphal ticks are about the size of poppy seeds, yet they carry the dangerous Lyme disease in their bites. Ticks are thought of as insects, but they are actually arachnids that are related to scorpions and spiders. Deer ticks are found all over the United States and in more than 60 other countries. These ticks attach to one’s skin through questing and are able to feed for several days on one host. If left undisturbed, they are more likely to transmit Lyme disease and other pathogens into one’s bloodstream.
Lyme disease is a bacterial infection that is transmitted by Ixodes ticks, more commonly known as deer ticks. These nymphal ticks are about the size of poppy seeds, yet they carry the dangerous Lyme disease in their bites. Ticks are thought of as insects, but they are actually arachnids that are related to scorpions and spiders. Deer ticks are found all over the United States and in more than 60 other countries. These ticks attach to one’s skin through questing and are able to feed for several days on one host. If left undisturbed, they are more likely to transmit Lyme disease and other pathogens into one’s bloodstream.
Recent Comments